Mental Health and Mesothelioma
While you’re dealing with the physical impacts of mesothelioma on your body, it’s important not to neglect your mental health. Learning healthy coping mechanisms can significantly improve your quality of life, serving as a resource you can draw upon through every step of the mesothelioma treatment process.
Home » Leading National Mesothelioma Law Firm » Mesothelioma Cancer » Mental Health and Mesothelioma
The Clinical Connection: Why Mental Health is Essential to Mesothelioma Care
Caring for your mental health after a mesothelioma cancer diagnosis is key to extending your life and preserving more quality time with your family. Findings in scientific studies like the following have shown a strong link between mental health and risk of death among cancer patients:
- Cancer patients who developed a mental health disorder were 51% more likely to die within the first three years after their cancer diagnosis, according to a recent study.
- An earlier study showed that patients who already had a mental health disorder also had a higher risk of death, even when accounting for treatment quality and cancer progression.
- Mindfulness practices such as meditation may reduce a cancer patient’s stress levels by roughly 23% on average.
- A 2020 National Cancer Institute study found that mental health treatment helped lung cancer patients live significantly longer, with a 26% reduction in overall mortality observed among a group of 50,000 veterans.

Tools for Assessing Your Mental Health
Mesothelioma patients can have their mental health evaluated by their medical providers. If you have concerns about your mental health, the National Comprehensive Cancer Network’s Distress Thermometer and Problem List are valuable tools to help assess your condition. Be sure to take the results to your next health care appointment.
You can download both documents to print and fill out using the links below.
Download Links:
What Are the Common Mental Health Conditions Associated With Mesothelioma?
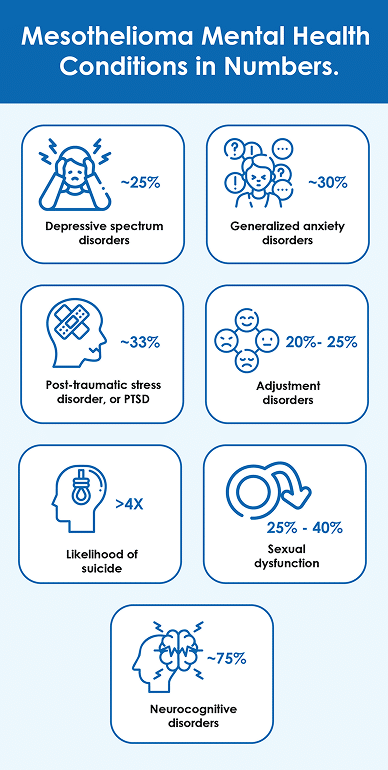
A variety of different psychiatric disorders affect as many as 4 in 10 cancer patients. Mental health conditions commonly associated with mesothelioma include:
- Depressive spectrum disorders: Roughly one quarter of all cancer patients experience major depression, or disruptive feelings of sadness, fatigue, and helplessness that last for two weeks or more.
- Generalized anxiety disorder: As high as 30% of mesothelioma patients experience significant anxiety symptoms, such as uncontrolled worrying, restlessness, or panic attacks.
- Post-traumatic stress disorder, or PTSD: As many as 1 in 3 mesothelioma patients show signs of PTSD, and caregivers often also experience trauma.
- Adjustment disorders: These overwhelming and uncontrollable emotional reactions to stressors affect 20 to 25 percent of cancer patients.
- Suicidal ideation: Cancer patients are more than four times more likely to die by suicide, though rates may be decreasing over time.
- Sexual dysfunction: Between 25% and 40% of cancer patients go through some changes in sexual functioning.
- Somatic symptoms: Many mesothelioma patients develop certain symptoms simply due to the fear of them, such as becoming nauseated when anticipating chemotherapy.
- Neurocognitive disorders: Up to 3 in every 4 terminal cancer patients may experience delirium, and a similar percentage may encounter “chemo brain” during treatment.


Mesothelioma Grief Counseling in the Aftermath of a Diagnosis
The natural human response to a devastating loss is grief. It’s understandable to feel overwhelming emotions after being diagnosed with a terminal illness. The following sections will discuss how to process grief, both in terms of death and the loss of life as it was once known.
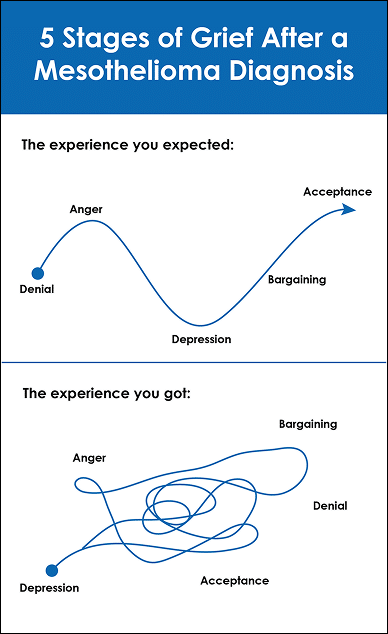
Mesothelioma Diagnosis and the 5 Stages of Grief
Medical professionals generally represent grief as a five-stage process. This framework can help you understand the complex emotions you’re feeling after a mesothelioma diagnosis, though the order in which you experience each element of grief might vary.
The following are the five stages of grief:
- Denial: A state of emotional numbness, shock, and refusal to believe that manifests as a defense mechanism when facing an overwhelming loss
- Anger: Feelings of rage and injustice that arise from the tragedy and unfairness of your situation
- Bargaining: A tendency to emotionally negotiate for a way to fix an unfixable situation, whether with fate or a higher power
- Depression: An overwhelming state of sadness, withdrawal, and loss of interest that develops when the reality of your loss sets in
- Acceptance: Means that while grief may remain, you’ve emotionally processed your loss as part of your life

The Dual Process Model for Mesothelioma: Balancing Loss and Restoration
Some critics of the five stages model have instead proposed a dual process framework that may more accurately portray the complex process of coping with a loss. This model can be particularly effective for those facing terminal illnesses like mesothelioma.
The dual process model explains that grief is a process of oscillating between confronting and avoiding two different types of grief-related stressors. Loss-oriented stressors center on directly processing death and its impact on you personally, while restoration-oriented stressors relate to the impacts on your life caused by the loss and what you have to do to respond to them.
The dual process may feel more relatable to someone experiencing complex, inconsistent grief, such as feeling fine one moment and devastated the next. It explains that taking breaks from the overwhelming weight of your emotions, or distracting yourself from feelings of loss, is normal and necessary.
Mesothelioma Coping Strategies For Patients and Loved Ones
The right coping mechanisms can help you and your family preserve your mental health after a mesothelioma diagnosis, improving your quality of life as you continue treatment.
5 Tips for Coping with a Mesothelioma Diagnosis
- Seek emotional support, whether through your loved ones, support groups, or individual counseling.
- Find a health care provider that has resources and programs dedicated to working with mesothelioma patients, including palliative and hospice care options.
- Practice mindfulness through meditation or yoga to help regulate your emotions.
- Maintain your physical health through regular exercise, sufficient sleep, and a healthy diet.
- Resist the urge to withdraw from others, and instead prioritize staying connected with your loved ones and community.
5 Tips for Coping with Death Anxiety
- Understand that it’s normal to feel anxious about dying, what comes after, and how your loved ones will manage without you.
- Recognize that your life matters and reflect on the impact you’ve had on others.
- Find meaning in something beyond yourself, focusing on your deepest values as you make the most of the time you have left.
- Confront your mortality head-on, facing your fears by exposing yourself to death-related content, planning your affairs, and thinking about how you want to be remembered.
- Shift your focus away from negative emotions and things you can’t control, and prioritize what you feel is truly important.
Download Mesothelioma Coping Strategies For Patients and Loved Ones in a PDF format to share or keep with you when you need it.
Veteran Mental Health Support for Asbestos-Exposed Service Members
Many military veterans were heavily exposed to asbestos during their service. Therefore, the U.S. Department of Veterans Affairs offers a variety of benefits to veterans diagnosed with mesothelioma, including mental health resources.
The Intersection of Military PTSD and Cancer Diagnosis
Being diagnosed with a cancer like mesothelioma can lead to PTSD-like symptoms and exacerbate how a veteran’s existing trauma affects their brain. In a 2015 study, roughly half of veterans interviewed six months after a cancer diagnosis reported it to be a significant traumatic stressor, with those with combat-related PTSD being more likely to agree.
Getting Help: VA Mental Health Services and Palliative Care
All veterans receiving VA health care can access Primary Care-Mental Health Integration, or PC-MHI, services. Through PC-MHI, a care manager can help you access the right treatments for your specific situation and symptoms.
You may also be eligible for palliative care, through which a team of medical providers, health care professionals, and others will work with you to help support you through living with mesothelioma.
You Are Not Alone: Cultivating a Network of Emotional Support
A mesothelioma diagnosis can affect every part of your life: physically, emotionally, and mentally. But, it’s important to remember that you don’t have to navigate this journey alone. Building a network of emotional support can make a meaningful difference in how you cope and heal.
Support can come from many places, including trusted family members, friends, mental health professionals, and mesothelioma support groups made up of others who understand what you’re going through. Many organizations and community programs also offer counseling, educational resources, and spaces to share your experiences in a safe and understanding environment.
If you’re struggling, reaching out is a powerful first step. Whether it’s speaking with a therapist, joining a support group, or simply opening up to someone you trust, help is available. Taking care of your mental health is just as important as addressing your physical health. And, you deserve compassion, connection, and care every step of the way.
