Mesothelioma Surgery
Surgery can be a large part of a patient’s experience with mesothelioma. Diagnostic surgery may be needed to obtain a biopsy to diagnose the cancer and therapeutic surgery to remove tumors to slow the spread of cancer. Palliative surgery may also be employed to make patients feel more comfortable.
Home » Leading National Mesothelioma Law Firm » Mesothelioma Cancer » Mesothelioma Treatment » Mesothelioma Surgery
Mesothelioma treatment may include various types of surgical procedures. In some cases, the biopsy that’s needed for the diagnosis may be obtained via a surgical procedure. Tumor-removing surgery may extend life in carefully selected patients, although not everyone is eligible.
Diagnostic Surgery for Mesothelioma
As part of the process of mesothelioma diagnosis, a biopsy is needed. This is a small sample of tissue that can be examined under a microscope by a pathologist. In certain cases, the necessary cells can be obtained through a minor procedure that is generally performed outside of the operating room.
- In a core needle biopsy, the sample is obtained using a needle inserted through the skin directly into the tumor. This may be possible if the tumor is located close to the skin.
- In some cases, a sample of fluid may contain enough cells for the pathologist to analyze. For pleural mesothelioma patients, the fluid may be obtained through thoracentesis (also known as thoracocentesis), a minor procedure in which fluid is drained from around the lungs using a needle or a catheter inserted through the chest wall.
A similar procedure called paracentesis is used in patients with peritoneal mesothelioma to drain excess fluid from the abdomen.
In other cases, however, a slightly more invasive surgery is needed to access the tumor in order to get a sample. These procedures are performed in the operating room, but are still considered relatively minor surgery.
- For pleural mesothelioma, video-assisted thoracoscopic surgery (also known as thoracoscopy) may be used. The thoracic surgeon makes small incisions in the chest wall between the ribs and inserts an instrument called a thoracoscope. Using a small camera, the surgeon can view the inside of the thoracic cavity on a video screen.
Surgical instruments can be passed through the scope to get the biopsy samples. In some cases, if the surgeon can’t access the tumor well enough through the tiny incisions, a procedure called thoracotomy may be used, which involves making a slightly larger incision to allow the surgeon to get the biopsy under direct visualization.
- For peritoneal mesothelioma, a similar procedure known as video-assisted laparoscopic surgery, or laparoscopy, can be used, involving inserting a laparoscope through small incisions in the abdominal wall.
If the surgeon needs greater access, then a laparotomy may be necessary, in which a larger incision is used to allow the surgeon to look inside the abdominal cavity directly.
Therapeutic Surgery for Mesothelioma
Certain patients may be candidates for therapeutic surgery, also known as tumor-removing surgery. In this type of procedure, the surgeon aims to remove as much of the cancer as possible, using different techniques for different types of mesothelioma. This is sometimes also known as potentially curative surgery, although mesothelioma is generally considered incurable. These procedures may extend life but are very unlikely to get rid of the cancer entirely.
Not all patients are candidates for these procedures. Patients must be in good overall health to be able to undergo a very invasive surgery. Additionally, certain characteristics of the tumor will determine whether surgery is a good option. Those with epithelioid tumors in an early stage are most likely to benefit.

For a surgeon, these are very technically demanding procedures. Because mesothelioma is relatively rare, most surgeons have not performed them very often. Receiving your treatment at a mesothelioma cancer center will give you access to a surgeon with the necessary experience to get the best possible results from the surgery.
Surgery is rarely used alone to treat mesothelioma. Rather, it’s generally part of a multimodality treatment plan, which may also include chemotherapy, radiation therapy, and/or immunotherapy. There are also a number of current clinical trials that involve testing the combination of other treatments with surgery, and some patients may choose to participate.
Each patient must make their own decisions about their cancer care. Research has shown that, in carefully selected patients, surgery can extend survival, which can buy more time with loved ones. At the same time, these are very invasive procedures, and patients will have lasting side effects from them. Some patients decide that they would rather focus on palliative treatment options rather than go through a major surgery.
Pleural Mesothelioma Surgery
Only patients with resectable tumors are candidates for tumor-removing surgery. Early-stage malignant pleural mesothelioma (stages 1 or 2) is generally considered resectable, and some stage 3 tumors may be resectable as well. Once the cancer has spread to lymph nodes or undergone metastasis, surgery is no longer an option. Additionally, patients with sarcomatoid tumors are not eligible for surgery because research has not shown a survival benefit for these patients.
In the past, the survival rates were higher with EPP than with P/D. However, due to advances in technique, the survival after P/D is now equivalent to that after EPP, and some studies have even reported that it’s slightly better. The median survival time after EPP is about 16 months, while after P/D, it’s about 22 months. Additionally, patients generally have a better quality of life following P/D because the lung is not removed.
There are two main types of tumor-removing pleural mesothelioma surgery:
- Extrapleural pneumonectomy (EPP) is the more invasive procedure. The surgeon removes the pleura (the lining of the lung) on the affected side, along with other tissues on that side, including the lung itself, part of the diaphragm, the pericardium (the sac around the heart), and sometimes other tissues.
- Pleurectomy/decortication (P/D) is a slightly less invasive procedure, although it’s still a major surgery. The pleura on the affected side is removed, and then the surgeon removes any visible tumor tissue. This procedure doesn’t remove the entire lung.
For these reasons, many oncologists and surgeons now consider P/D to be the better of the two surgical options for the management of malignant pleural mesothelioma, but your doctor will discuss with you what they believe would be the best treatment in your specific case.
Some surgeons incorporate intraoperative administration of chemotherapy, known as hyperthermic intrathoracic chemotherapy (HITHOC), into the surgical procedure. After removing as much cancerous tissue as possible, a heated solution of chemotherapy drugs is infused into the thoracic cavity. It’s left for a period of time and then washed out. This is a relatively new procedure for pleural mesothelioma, but research indicates that it may be effective. Most patients receive follow-up treatments after surgery, to target cancer cells that may not have been removed by the procedure. The treatment plan may include chemotherapy (known as adjuvant chemotherapy), immunotherapy and/or radiation therapy (also known as radiotherapy).
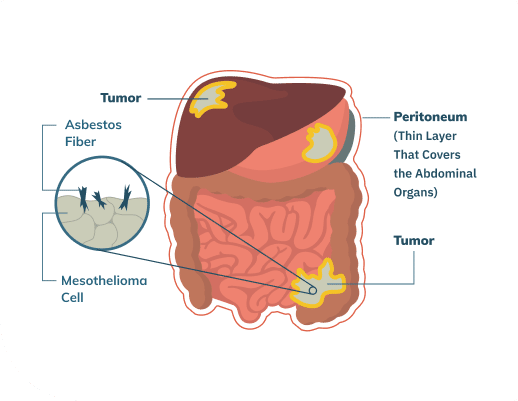
Peritoneal Mesothelioma Surgery
In general, there’s one type of surgery that’s preferred for patients with peritoneal mesothelioma. Patients with epithelioid tumors whose disease has not metastasized are generally candidates for this procedure, which is called cytoreductive surgery (CRS). The surgeon removes as much tumor tissue as possible from the abdomen, a process known as debulking.
This generally involves removing many parts of the peritoneum (the membrane around the digestive system), and sometimes other organs, such as the gallbladder, spleen, and/or parts of the intestine. The specifics of the tissue removal depend on where visible tumors are present.
Hyperthermic intraperitoneal chemotherapy (HIPEC) is usually also used as part of the procedure. After CRS, a heated solution of chemotherapy drugs is infused into the abdominal cavity, left for a period of time, and then washed out. The combined procedure is known as CRS-HIPEC.
CRS-HIPEC can offer a significant survival benefit in carefully selected patients. Some centers have reported 5-year survival of up to 44% following CRS-HIPEC. However, the procedure does carry a risk of mortality (up to almost 5%) and has significant side effects. Additionally, patients with sarcomatoid or biphasic tumors or whose cancer has already metastasized are not candidates for the procedure.
Palliative Surgery for Mesothelioma
Surgery can also be used for palliative care. A palliative procedure may help to make the patient more comfortable and reduce the symptoms of the cancer, which improves quality of life. There are several palliative treatment options.
Thoracentesis, described earlier, may help to control symptoms like shortness of breath that can be caused by a pleural effusion, or fluid buildup around the lungs. For peritoneal mesothelioma patients, paracentesis may help with discomfort caused by ascites, or fluid buildup in the abdomen.
Pleurodesis may help pleural mesothelioma patients who experience repeated pleural effusions. In this procedure, the two layers of the pleura are surgically adhered to each other. The doctor uses a thoracoscope to insert a medication (such as medical talc) between the layers of the pleura, which causes them to adhere to each other.
In partial pleurectomy, part of the pleura is removed in order to improve patient comfort. It may be used for some patients who experience repeated pleural effusions, but studies show that pleurodesis provides better results with fewer side effects, and so it’s generally preferred.
